What is Pain?
(And Why Yours Might Not Mean What You Think)
"Pain is pretty simple, right? Something breaks, it hurts. Something heals, it stops."
Freddie: "I'm about to ruin pain for you. In the best possible way."
Pain is not a damage detector
Here's the thing most people get wrong.
Pain doesn't measure how much damage is in your body.
Pain measures how much your brain thinks you need protecting.
That's a big distinction.
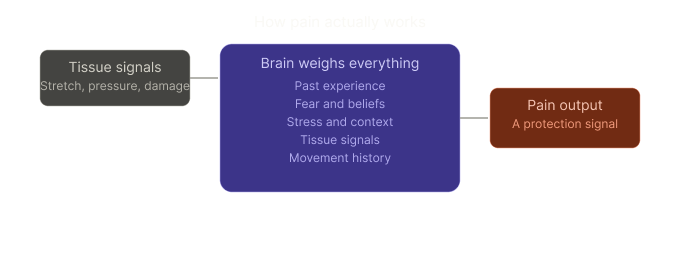
Professor Lorimer Moseley — one of the world's leading pain scientists — puts it brilliantly: pain is an output of the brain, not an input from the tissues. Your tissues send signals. Your brain decides whether to produce pain based on a whole lot of other information — stress, fear, context, past experience, what you believe about your body.
This is why:
Soldiers in battle don't feel bullet wounds until after the fight
Paper cuts hurt more than much bigger injuries
The same movement can feel fine one day and agonising the next
People can have severe back pain with nothing structurally "wrong" — and vice versa, a completely wrecked-looking MRI with zero pain
Pain is your brain's best guess at whether you need to stop and pay attention. It is not a reliable measure of how damaged you are.
Damage can exist without pain. Pain can exist without damage.
The brain decides — not the tissue.
The smoke alarm analogy
Moseley uses a great analogy: pain is like a smoke alarm. A smoke alarm doesn't detect fire — it detects smoke. And sometimes it goes off when you're just making toast.
Your nervous system is the same. It's set up to be protective, not accurate. It would rather give you a false alarm than miss a real threat. After an injury, or under chronic stress, or when you're anxious about your body — the alarm becomes hypersensitive. It starts going off with less and less smoke.
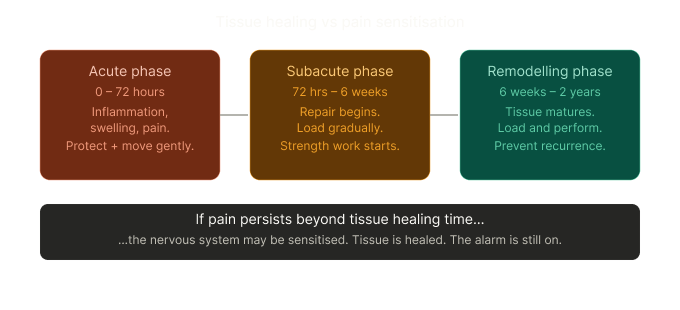
This is called central sensitisation — and it explains why chronic pain can persist long after the original injury has healed.
"So the fire might be out, but the alarm is still screaming?"
Freddie: "Exactly. And the answer isn't to ignore the alarm — it's to recalibrate it."
The Protectometer: what turns pain up or down
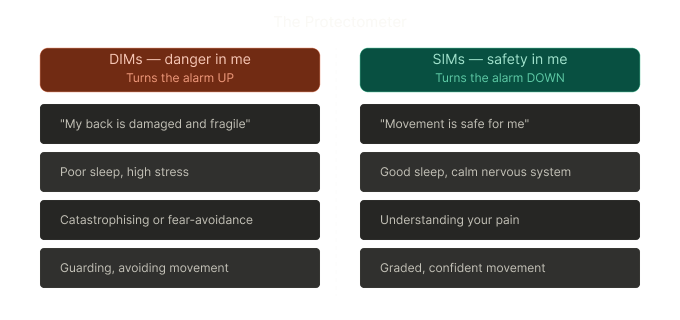
Moseley developed a tool called the Protectometer. The idea is simple: your brain is constantly running a calculation. On one side, things that make it feel safe. On the other, things that make it feel threatened. When the threat side tips the scales — pain goes up.
These inputs are called DIMs and SIMs.
This is why two people with identical injuries can have completely different pain experiences. It's not about who's tougher. It's about what their nervous system has learned, and what it currently believes about safety.
At The Movement Co, a big part of what we do is help shift the balance toward SIMs — through education, graded movement, and rebuilding confidence in your body.
So where does actual tissue damage fit in?
Great question — because tissue damage does matter, especially early on. This is where the mechanism of injury comes in.
When you get hurt, the type, direction, and force of the injury tells us a lot about what structures are involved. A sudden twisting ankle tells a different story to a gradual onset of knee pain after increasing your running mileage. We call this the mechanism of injury (MOI) — and it's the first question we ask.
Understanding the MOI helps us:
Know which tissues are likely involved (ligament vs tendon vs bone vs nerve)
Understand whether the injury is acute (fresh) or chronic (long-standing and sensitised)
Plan treatment that matches what the tissue actually needs — not just where it hurts
The tissue healing timeline matters too. Different structures heal at different rates, and pushing too hard too early — or doing nothing for too long — both cause problems.
What this means for how we treat you
At The Movement Co, we hold both of these truths at the same time:
Tissue matters. We assess it properly, treat it appropriately, and load it progressively.
The nervous system matters equally. We don't just fix the structure — we help your brain feel safe moving again.
That's why our sessions combine hands-on treatment with education and graded rehab. Knowing why you're in pain is often the first step to reducing it. Research consistently shows that people who understand pain science recover faster and return to activity more confidently.
"So you're basically treating the body AND talking the brain down off a ledge."
Freddie: "That's... actually a perfect description. Yes."